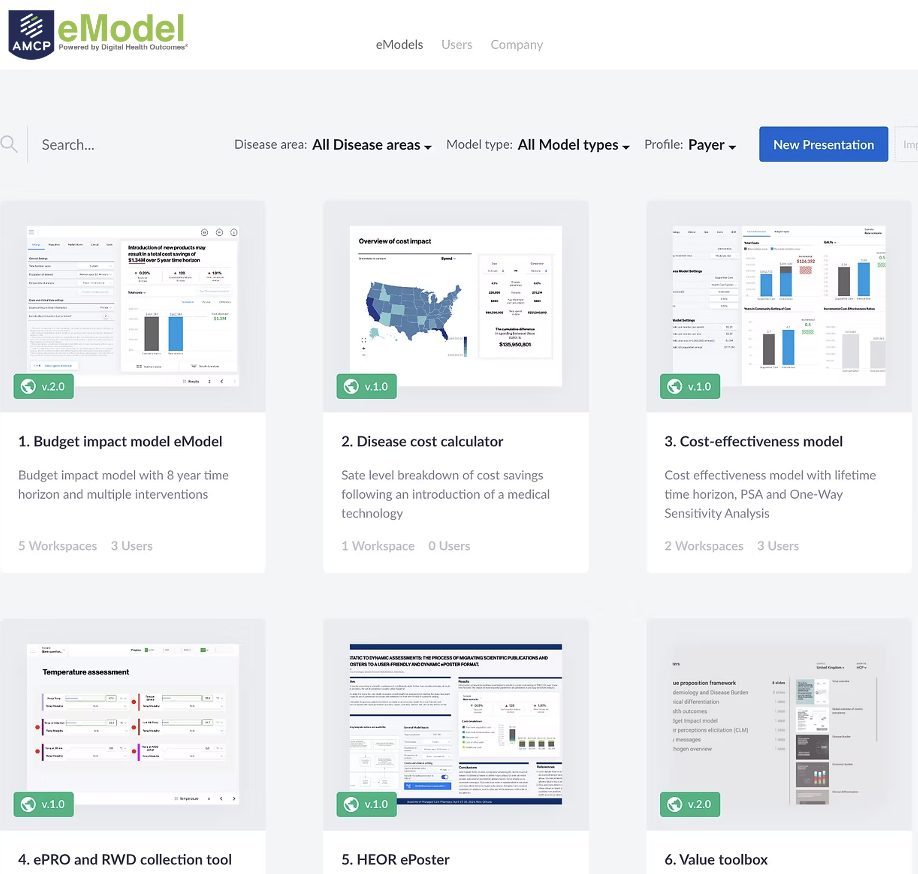
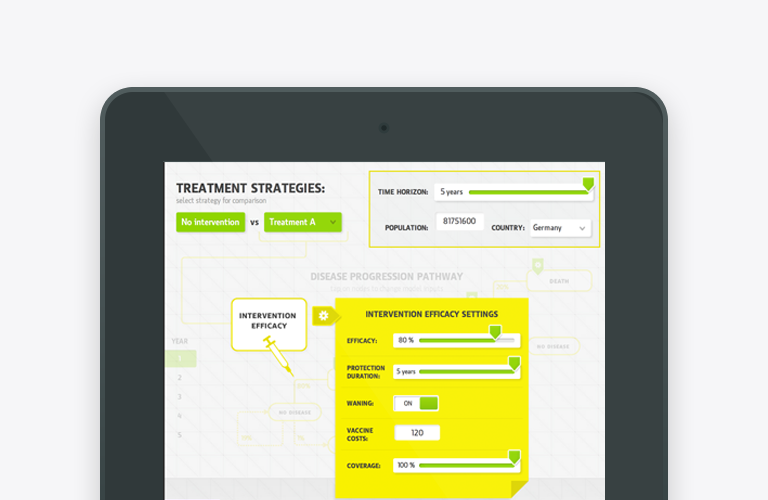
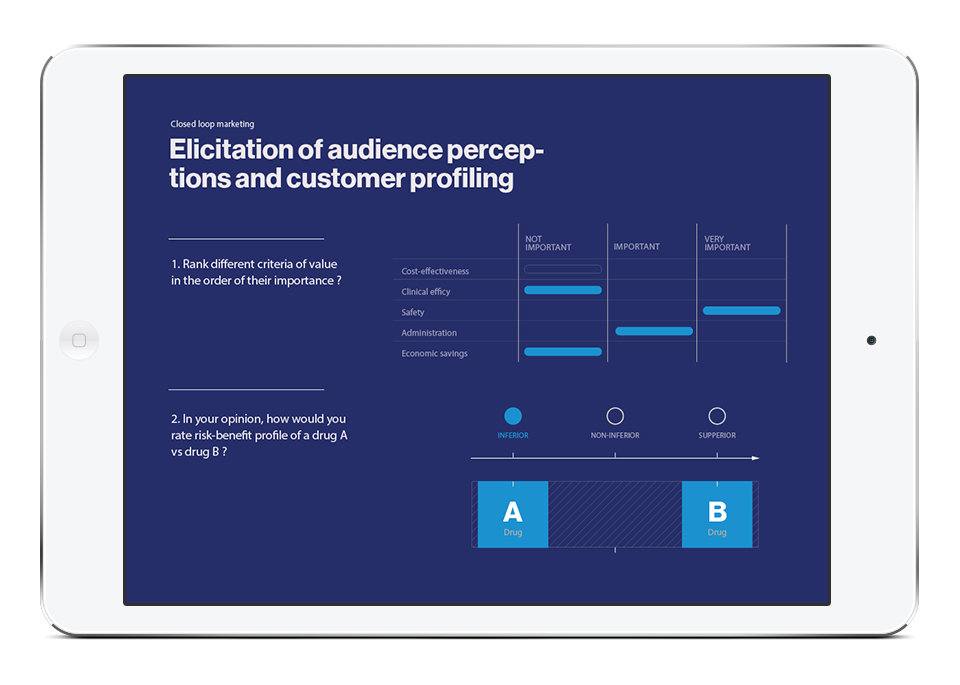
In the current age of rapidly developing informational technologies they are literally impacting more and more spheres of social life, and Healthcare has not been an exception. Such notions as Digital Marketing and eDetailing have infiltrated pharmaceutical and life science industries long ago and reliably anchored within. This process quickly included the products of fast-growing market of mobile/tablet devices and other gadgets. Thus, new user-friendly application development opportunities were discovered, often accompanied by cloud-based technologies, which are globally accessible and synched.
Such new abilities to link patients with doctors using online networks and other modern technological opportunities greatly improve patient awareness about existing drugs and treatment pathways; however there remains a number of obstacles, which interfere with the rapid deployment of healthcare innovations into our daily life and in this article we will identify and discover their meaning.
- Privacy and security. Healthcare service providers and software developers usually need to determine data storage conditions and undertake all the necessary actions in order to make sure that the information is subject to all possible measures of oversight and control. It is complicated by the fact of increasing complexity of protected information management, due to large number of interconnections and inter-dependencies among various products and industry participants.
- Integration. Effective integration of digital solutions within already existing infrastructure is crucial. This process incorporates both the technological and the human factors of care delivery.
- Data storage and exchange. It is recognized, that for a true digital revolution of healthcare, it is necessary for the many different IT, mobile/digital systems and networks to interact and exchange data with one another. And the current rise of data-driven solutions in healthcare is resulting in the creation of large volumes of clinical, personal, operational and institutional data that is growing rapidly.
- Scalability. Increasing number of users raises the amount of data produced, as well as the required number of connections involved. It also means that are greater burdens on networks, an increased potential for security breaches, as well as difficulties integrating with other care provisions.
- Accessibility. The manner and style in which a user interacts with the technology is a significant factor in terms of adoption. It is critical that a solution can be easily integrated into existing care pathways without necessitating additional burden or complication to the user.
- Quality. Presumably medical applications should be peer-viewed by clinical experts and that regulatory measures should be increased in order to safeguard the quality of care. This would allow healthcare professionals to be made aware which digital solutions lack evidence and professional involvement in their design and development.
- User engagement. Maintaining engagement with digital solutions is essential to ensure that they continue to be useful. Developers and solution providers must therefore design systems in ways that continue to engage with users and to encourage long-term adherence.
- “Consumerisation” of healthcare. Tech-savvy patients are used to managing so many aspects of their lives with the assistance of technology, that they are beginning to demand to do the same with their health. As a result providers need to consider new ways of engaging and providing access to services, which means laterally diversify into offering technology to support their core competencies.
- Liability and legal aspects. The legal and regulatory landscape surrounding digital and mobile health solutions is still very much in its infancy, leaving considerable uncertainty for care providers and solution developers.
- Cost implications. The implementation of mobile digital solutions is often seen as a double-edged sword when it comes to the issue of costs. Problems arise when there is a need to change workflows and clinical pathways in order to incorporate the technology. In this case the short-term expenditure necessary for the implication (e.g. equipment, staff training, policy changes, changes to working practices etc.) are often viewed by commissioners as prohibitive, rather than as precursory enablers of long-term investments.
- Health economics. Many secondary care organisations around the world are reimbursed for their services, either by central funding or insurance payments, based upon the number of patients they treat, as well as number of key, care quality criteria. At present many of these methods for calculating reimbursements are actually prohibitive of digital health solutions, despite their ability to improve patient outcomes, reduce hospital visits and reduce readmissions.
- Government regulation and policy. With the scope for life-prolonging medical intervention now virtually limitless – and thus spending on it being potentially limitless as well – there are moral and practical questions about its availability and distribution which every democratic society has to address.
It is yet a well-known fact, that implementation of modern technologies into healthcare greatly improves our life standards and increase lifespan. However, such implementation rapidity may vary and it directly depends on the identification and solution of the related problems and obstacles.
Article was written based on the DHO team experience and literature review.